As health care professionals, we all have a role to play in slowing the spread of the coronavirus by following some advice shares by scientific groups and health organizations to help limit infections and slow down the spread of the virus.
This is the responsibility of all world citizens, thanks to collective actions, to limit the spread of the virus.
Purgo Biologics wants to share simple protocol to help dental professionals to work in safe conditions for themselves, their staff, and their patients.
These recommendations outlined are subjected to change as the sanitary situation evolves.
Always be cautious, focused, and follow the recommendations issued by the local health authorities or recommendations of the regional dental
Our priority, Your Safety!
[Before starting the lecture of the following article, please note, that the following contents are based and reviewed from a selected source of scientific reports and official government statements.]
The COVID -19?
COVID-19 is the infectious disease caused by the most recently discovered coronavirus. This new virus and disease were unknown before the outbreak began in Wuhan, China, in December 2019. COVID-19 is now a pandemic affecting many countries globally.
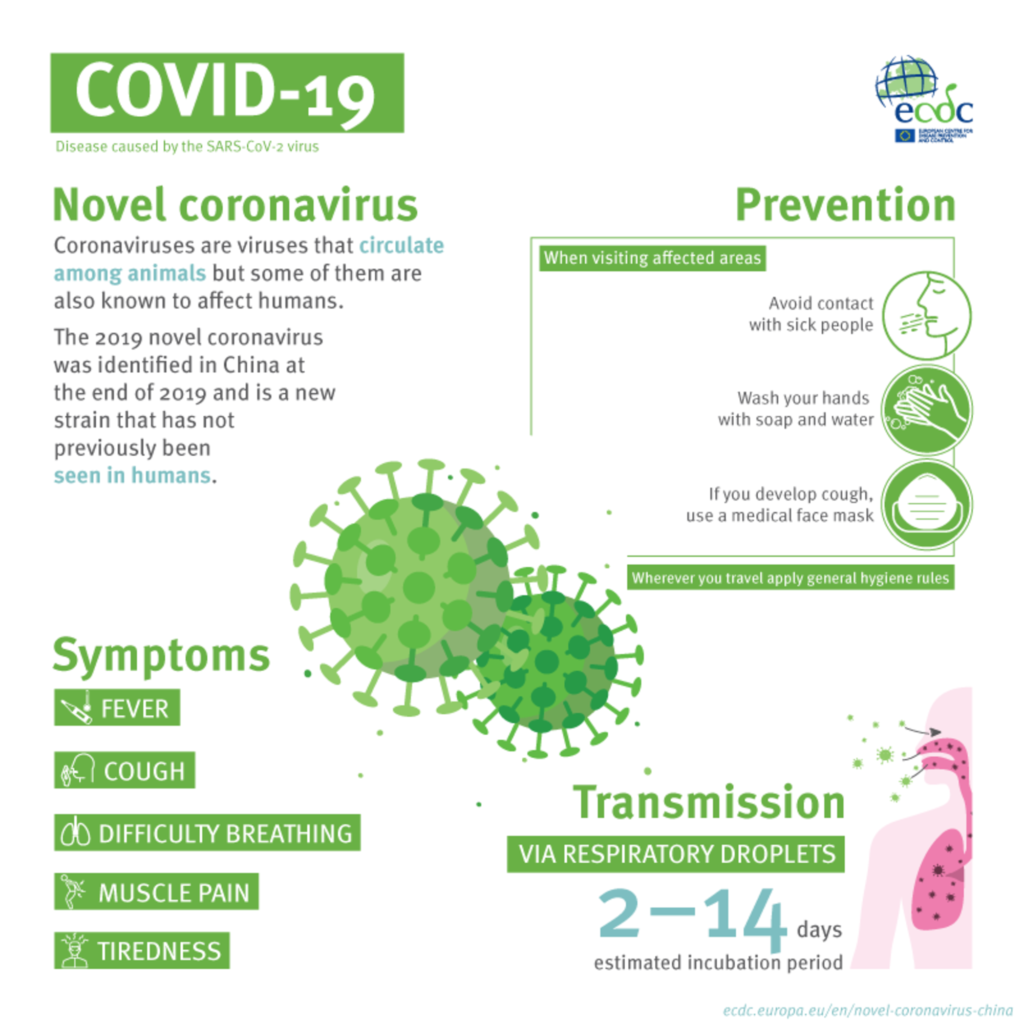
How does it spread?
The scientist’s research tends to believe that animals are the source, we can see the virus spreading from human-to-human transmission.
The scientific evidence confirms that COVID-19 is spread by droplets. When an infected person coughs, sneezes or talks, they may generate droplets containing the virus. These droplets are too large to stay in the air for long, so they quickly settle on surrounding surfaces.
There is also evidence that the COVID-19 virus can last on surfaces – especially plastic or metal – for up to 3 days. This is why advice to avoid catching COVID-19 has focused on handwashing with soap, the use of alcohol-based hand sanitizing gels and keeping a distance from people who are symptomatic.
Some recent studies have suggested that COVID-19 may be spread by people who are not showing symptoms.
Symptoms may appear 2-14 days after exposure to the virus. People with these symptoms may have COVID-19:
Cough – Shortness of breath or difficulty breathing – Fever – Chills – Muscle pain – Sore throat- New loss of taste or smell
This list is not all inclusive. Other less common symptoms have been reported, including gastrointestinal symptoms like nausea, vomiting, or diarrhea.
Watch video from the World Health Organization about the Covid-19 and spread:
PRECAUTIONS & RECOMMENDATIONS
Avoid every light procedure, non-urgent dental surgeries, and dental visits of your patients. The services provided by a dentist and patrician should be limited to the emergency visits only during the crisis to keep in safety the patients, the health worker staff, and the specialist.
If sick and Symptoms: Stay at home!
In the case, you or your staff have developed symptoms while at work, send the staff and yourself at home. If you feel sick and have a respiratory infection, do not try to work and contact immediately the recommended emergency center of your country.
Don’t forget the teledentistry and teleconferencing.
You can contact all your schedule patient trough a telephone screen to check the signs or symptoms of respiratory illness (fever, cough, shortness of breath). Delay, if possible, every dental care emergency until an infected patient has entirely recovered from the respiratory infection and provide them home care instructions and any appropriate pharmaceuticals help.
What to do If a patient without the COVID-19 came to my facility?
– Check if your patient has the COVID-19 through a form and questions him about the presence of symptoms of a respiratory infection and travel to areas experiencing transmission of COVID-19 or contact with possible patients with COVID-19. You can find in this article a form to help you with the check-in of the patient.
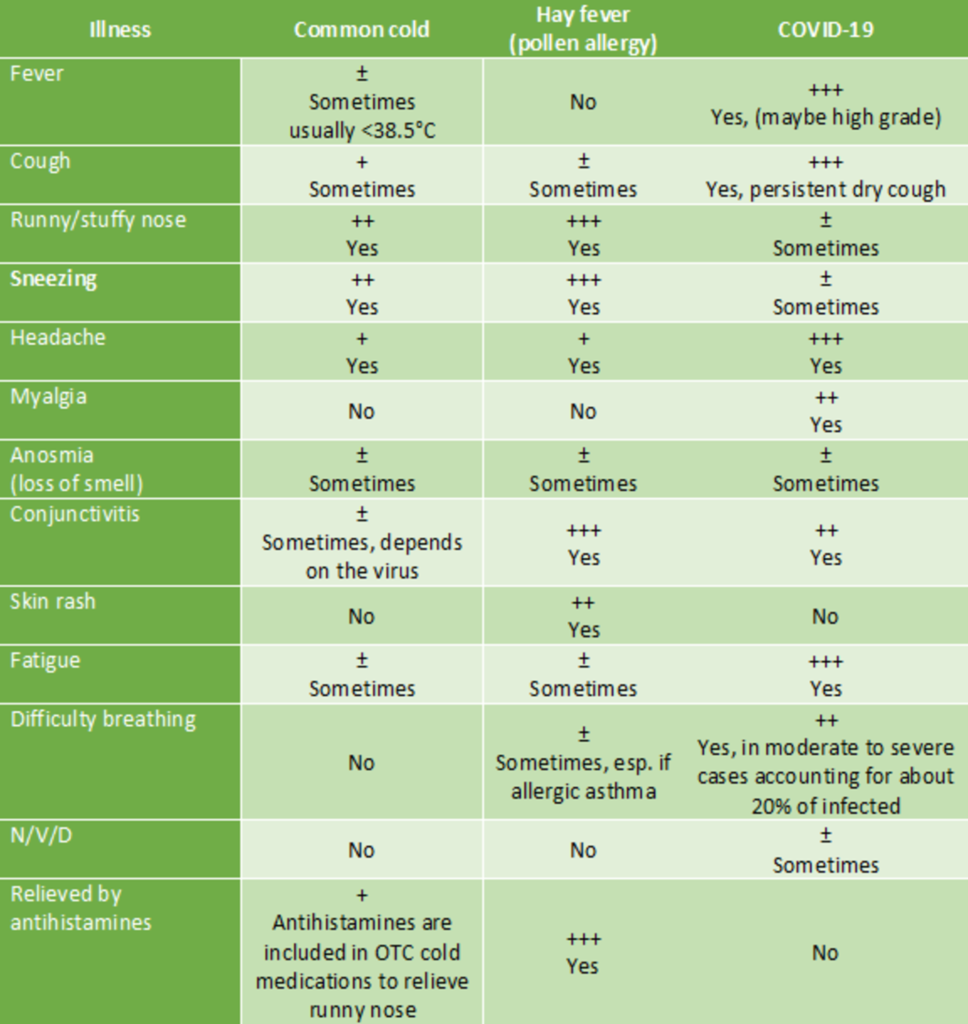
(source: European Centre for Disease Prevention and Control)
– Control the temper of your patient, he should be afebrile:
Normal: 36.5–37.5 °C (97.7–99.5 °F)
Hypothermia: <35.0 °C (95.0 °F)
Fever: >37.5 or 38.3 °C (99.5 or 100.9 °F)
Hyperthermia: >37.5 or 38.3 °C (99.5 or 100.9
– Avoid aerosol-generating procedures whenever possible. Avoid the use of dental handpieces and the air-water syringe. The use of ultrasonic scalers is not recommended during this time. Prioritize minimally invasive/atraumatic restorative techniques (hand instruments only).
– If aerosol-generating procedures are necessary for emergency care, use four-handed dentistry, high evacuation suction and dental dams to minimize droplet spatter and aerosols.
What to do If a patient with the COVID-19 came to my facility?
After the check of your patients, in this case, if you suspect or confirm that the patient has the COVID-19, you should take the following actions:
– Defer dental treatment
- Give the patient a mask to cover his or her nose and mouth, (if it’s not the case) and avoid every physical contact with the other patients, your staff, and you.
- If not currently sick, send the patient home and instruct the patient to call the recommended emergency center for coronavirus for advice and recommend him a teledentistry consultation.
- If he is sick (for example, has trouble breathing) refer the patient to a medical facility.
What should I do if the patient has the COVID-19 and his in need of a dental emergency necessary?
- Take some Airborne Precautions (an isolation room with negative pressure relative to the surrounding area and use of an N95 filtering disposable respirator for persons entering the room).
- The dental treatment should be provided in a hospital or other competent facility to handle the COVID-19.
Protect yourself with the highest level of personal protective equipment (PPE):
- Wear gloves, a gown, eye protection wear gloves, a gown, eye protection (i.e., goggles or a disposable/reusable face shield that covers the front and sides of the face), and an N954 or higher-level respirator during emergency dental care for patients without COVID-19.
- Removed disposable respirators and discarded them after exiting the patient’s room or treatment area.
- Clean and disinfect every reusable eye protection. If only disposable eye protection, you should discard it after every use.
- If soiled, change the gown, remove and discard the gown in a waste or linen container before leaving the patient room or treatment area. Or it should be transported to the temporary storage area of the dental clinic/ medical institute timely
- If a respirator is unavailable, use a combination of a surgical mask and a full-face shield (cleared and recommended by your country government).
- Surgical masks should be removed and discarded after exiting the patient’s room or care area.
- Change surgical masks during patient treatment if the mask becomes wet.
- Clean, disinfect, or discard the surface, supplies, or equipment located within 2m of symptomatic patients.
- Use products with approved by the regulation organism (like EPA) and emerging viral pathogens claims.
- Screen all DHCP at the beginning of their shift for fever and respiratory symptoms. Document shortness of breath, new or change in cough, and sore throat. If they are ill, have them put on a facemask and leave the workplace.
Your clinic should be clean, you should take effective and strict disinfection measures in the clinical settings and public areas, don’t forget the COVID-19 can survive 24 hours on the surface. You can use the following cleaners such as 0.1% sodium hypochlorite, 0.5% hydrogen peroxide, or 62-71% ethanol have all been shown to be effective.
Source: DOCS EDUCATON
If you want more details, you can directly download the report from the World Health Organization for more information at this address:
Also you can watch the video from the World Health Organization regarding seven steps to prevent the spread of the virus:
Don’t forget to visit the following References Institutes:
CDC – FDI – RKI – FOPH – WHO – ECDC
Sources and reference used to prepare this article:
WHO Link 1 – Link 2
References
WHO Director-General’s opening remarks at the media briefing on COVID-19 – 11 March 2020. 2020.
Versaci, M.B., CDC Reminds Clinicians to Use Standard Precautions, Recommends Isolating Patients with Coronavirus Symptoms. . American Dental Association, February 7, 2020.
Peng, X., et al., Transmission routes of 2019-nCoV and controls in dental practice. Int J Oral Sci, 2020. 12(1): p. 9.
Meng, L., F. Hua, and Z. Bian, Coronavirus Disease 2019 (COVID-19): Emerging and Future Challenges for Dental and Oral Medicine. J Dent Res, 2020: p. 22034520914246.
To, K.K., et al., Consistent detection of 2019 novel coronavirus in saliva. Clin Infect Dis, 2020.
Fang, L.S.T., Coronavirus and the Dentist, 2020, DOCS Education.


 Italia
Italia
